Advantages of Loupes and Lights for Dermatology

ErgoPractice News – April 2023
By Jin Chang PhD
jchang@surgitel.com
Summary
Just as any clinician, dermatologic surgeons are susceptible to work-related ailments due to their non-ergonomic working posture. A survey of Mohs surgeons and workplace ergonomics found that 90% of respondents reported a degree of musculoskeletal symptoms or injuries.1,2 The most common ailments are pain and stiffness in the neck, shoulders, and lower and upper back, as well as headaches.1-3,6 For the sake of getting a better view, the surgeon will often put themselves in ergonomically disagreeable positions. The prime working years for a dermatologic surgeon also tend to coincide with the age that presbyopia tends to begin, making magnification even more important. In this issue of ErgoPractice News, we will be discussing the benefits of magnification and headlights for dermatologic surgeons, and the different options that are available.
Benefits and Importance of Magnification for Dermatologic Surgeons
Most dermatologists find some type of magnifying system useful in their practice. Magnification allows enhanced visualization of fine anatomic details and precise suture placement. While higher magnification will produce a larger image, it also will reduce the field of view and depth of field.3 There are many examples of improved surgical quality and outcomes with magnification in other specialties. In one study, Hart and Hall4 illustrated the advantage of magnification in laceration repairs in the emergency department. Schoeffl et al5 demonstrated that the microsurgical success of fine surgical procedures was directly related to optical magnification strength when comparing the unaided eye, surgical loupes, and an operating microscope. By utilizing magnification that promotes a safer neck angle and a more ergonomic posture, it minimizes eye and musculoskeletal strain, allowing you to have a pain free career from bad posture (Figure 1). Magnification has been shown to improve posture in dental literature, a specialty with similar occupational risk factors to dermatologic surgery.3

Figure 1: Comparison of how magnification can impact ergonomics
Magnification Options
Loupes

Figure 2: SurgiTel’s family of loupes
Since the 1980’s the use of loupes (Figure 2) in dermatological surgery has become more popular.1,7 Dermatologists found that loupes at a magnification of 3.0x to 4.0x were the most useful as a diagnostic tool. Higher magnifications failed to yield additional clinically useful detail. Lower powered loupes of 2.0x to 2.5x were found to be useful as surgical aid, but provided less than optimal magnification for diagnostic purposes.7 In a 2022 survey, the most frequently cited benefit of using loupes was improved acuity/vision. Additionally when rating surgical outcomes and the use of loupes, most respondents felt that they improved their surgical outcomes by “a great deal”.1 Other benefits that the 2022 study found included improved blade and suturing precision, identification of bleeding points, and improved posture.1 Similar findings were replicated in other studies.8,9,10 Another benefit of using loupes is the advantage of eye-protection. SurgiTel has patented pantoscopic tilt of frame and/or lenses to help give a steeper declination angle and can eliminate gaps between the face and the bottom edge of the lenses to give better eye protection. Stationary working positions and neck flexion are risk factors for strain and injuries that dermatologic surgeons often encounter,2,3 this is why SurgiTel designed our loupes to be able to allow clinicians to make minor adjustments in their posture to minimize the risk of injury.
Dermatoscope

Figure 3: Example of a dermatoscope
A dermatoscope (Figure 3) is a magnifying tool about the size of a small computer mouse that uses light to give a bigger, clearer picture of a skin lesion. The dermatoscope has a wide range of magnification options, the most common is 10.0x. During an examination, dermatologists put the dermatoscope on or slightly above skin lesions and look for specific patterns, shapes, colors and structures not visible to the naked eye to get a better sense if a spot is worrisome. While it is small and mobile, it has minimal benefits to the dermatologic surgeon during surgery because it is handheld and has a small field of view.3 Another drawback is that when using it, you are put into a nonergonomic posture (Figure 4). Figure 5 shows the stress the neck can be put under when in a nonergonomic position.

Figure 4: Example of posture when using a dermatoscope
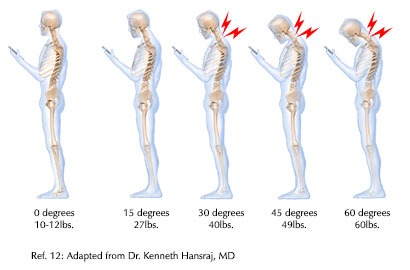
Figure 5: Neck posture and spinal stress
Magnification Stand
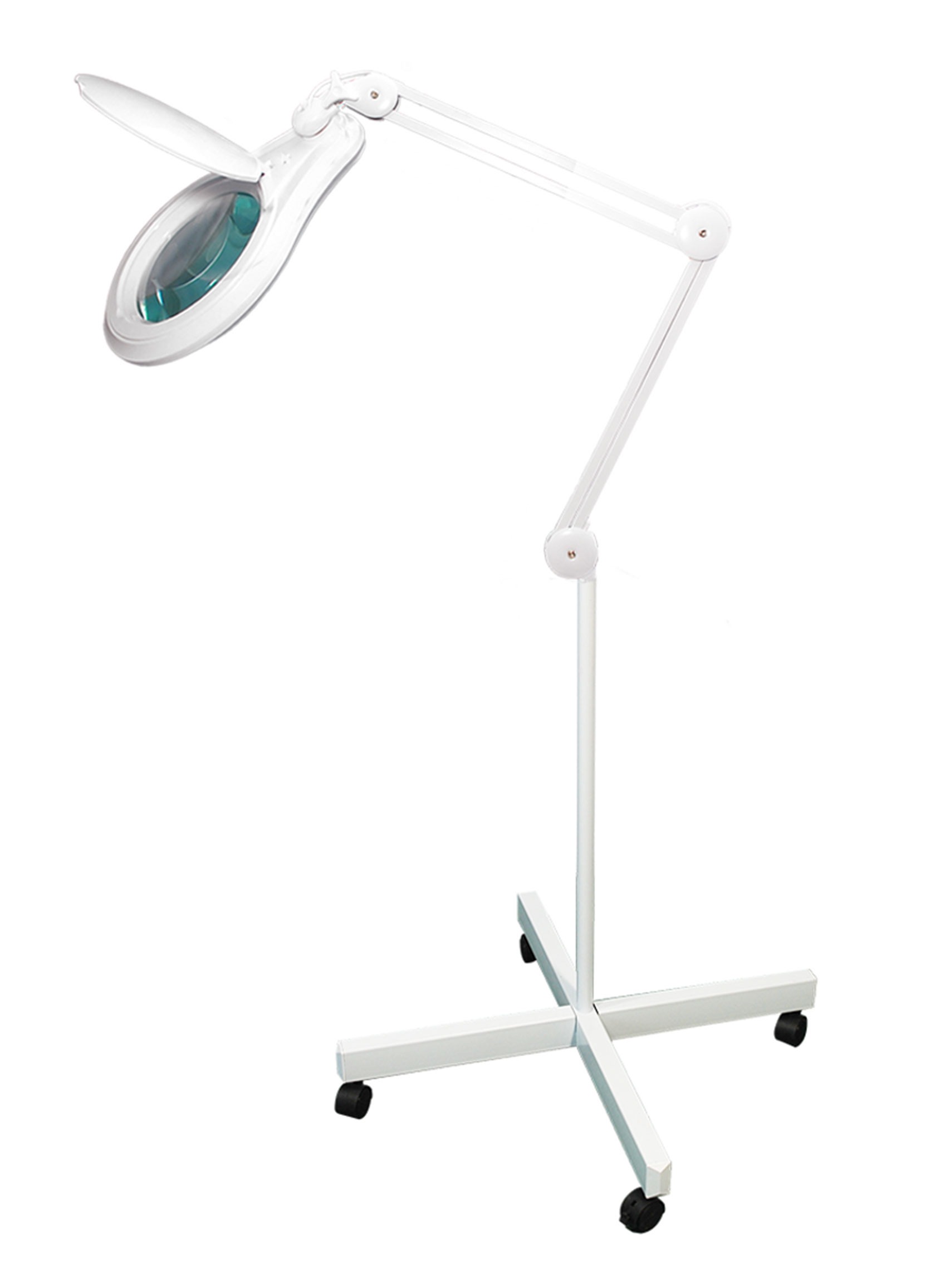
Figure 6: Example of a magnification stand
Source: BoliOptics
The magnification stand comes as a large magnification lens with a flexible arm attached to a stand (Figure 6). It’s a basic magnification tool and does not need to be worn; however, the stand is not easily portable and may be cumbersome to use.3 When using the magnification stand, you and your client can be put in uncomfortable and awkward positions. If you are hunched over the stand in a non-ergonomic position to get a better view, you are at risk of musculoskeletal pain or injuries. The magnification stand also needs to be adjusted every time you want the view to change, taking up valuable time and interrupting your work flow.
LED Headlights
SurgiTel offers contrast enhancement filters that enhance the image of veins (Figure 7). Cross-polarizing filters block light reflected from the stratum corneum, the outermost layer of the epidermis, and allows the clinician to see the internal structure of the skin.11 Color accuracy is needed in a dermatological LED headlight to see specific patterns, shapes, colors and structures of certain skin lesions for a proper diagnosis. In order to see best, a light must also produce a uniform beam. If a beam is uneven, we will perceive a spot of overly bright glare in the center, with a dim lack of detail on the periphery. SurgiTel LED headlights have patented optics to create a superior beam quality, we also have a coaxial design to produce a shadowless work space.
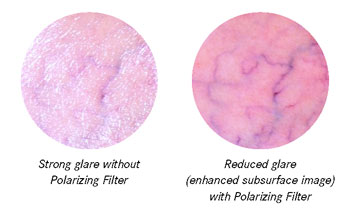
Figure 7: Example of effectiveness of cross-polarization filter
Two new surgical LED lights include lightweight surgical options and temperatures:
- Surgical Mini LED light – 5700K (Figure 8 Left)
- One of the lightest surgical lights on the market at 14.6 grams
- 100,000 lux
- 40% brighter than the Odyssey Mini Cool LED (5700K) light
- Improved battery pack with up to 12 hours of battery life
- Frame- or Headband-mounted options
- Surgical Headband LED 2.0 – 6500K (Figure 8 Right)
- 20% brighter than the previous Surgical Headband LED 1.0 (6500K) lights
- Improved battery pack with up to 12 hours of battery life
- Frame- or Headband-mounted options

Figure 8: Surgical Mini LED (Left) and Surgical Headband LED 2.0 (Right)
References
- Hunt, William T., Iqra Ashraf, and Toby G. Nelson. “A Multinational Survey Characterizing the Use of Surgical Magnifying Loupes in Dermatological Surgery.” Skin Research and Technology 28, no. 3 (May 2022): 439–44. https://doi.org/10.1111/srt.13144.
- Liang, Christine A., Vicki J. Levine, Stephen W. Dusza, Elizabeth K. Hale, and Kishwer S. Nehal. “Musculoskeletal Disorders and Ergonomics in Dermatologic Surgery: A Survey of Mohs Surgeons in 2010.” Dermatologic Surgery 38, no. 2 Part 1 (February 2012): 240–48. https://doi.org/10.1111/j.1524-4725.2011.02237.x.
- Chodkiewicz, Hubert M, and Aaron K Joseph. “Magnification for the Dermatologic Surgeon.” Cutis 99, no. 6 (June 2017): 413–17. https://cdn.mdedge.com/files/s3fs-public/Document/June-2017/CT099006413.PDF.
- Hart, Raymond G., and Jennifer Hall. “The Value of Loupe Magnification: An Underused Tool in Emergency Medicine.” The American Journal of Emergency Medicine 25, no. 6 (July 2007): 704–7. https://doi.org/10.1016/j.ajem.2006.11.039.
- Schoeffl, Harald, Davide Lazzeri, Richard Schnelzer, Stefan M. Froschauer, and Georg M. Huemer. “Optical Magnification Should Be Mandatory for Microsurgery: Scientific Basis and Clinical Data Contributing to Quality Assurance.” Archives of Plastic Surgery 40, no. 02 (March 2013): 104–8. https://doi.org/10.5999/aps.2013.40.2.104.
- Esser, Adam C., James G. Koshy, and Henry W. Randle. “Ergonomics in Office-Based Surgery: A Survey-Guided Observational Study.” Dermatologic Surgery 33, no. 11 (November 2007): 1304–14. https://doi.org/10.1111/j.1524-4725.2007.33281.x.
- Epstein, Ernst. “Magnifiers in Dermatology: A Personal Survey.” Journal of the American Academy of Dermatology 13, no. 4 (1985): 687–98. https://doi.org/10.1016/s0190-9622(85)70212-5.
- Wei, Chen, and Albert Y. Wu. “Surgical Loupe Usage among Oculoplastic Surgeons in North America.” Canadian Journal of Ophthalmology 53, no. 2 (April 2018): 139–44. https://doi.org/10.1016/j.jcjo.2017.08.011.
- Wajngarten, Danielle, Ana Carolina Botta, and Patrícia Petromilli Garcia. “Magnification Loupes in Dentistry: A Qualitative Study of Dental Students’ Perspectives.” European Journal of Dental Education 25, no. 2 (May 2021): 305–9. https://doi.org/10.1111/eje.12605.
- Hayes, Melanie J., Adam A. Rogers, Janet Chuanon, Thomas Tan, Ivan Lai, and Elisha Yong. “Dental and Oral Health Students’ Perceptions of Loupes.” International Journal of Occupational Safety and Ergonomics 27, no. 1 (March 2021): 136–43. https://doi.org/10.1080/10803548.2019.1574110.
- Kaliyadan, Feroze. “The Scope of the Dermoscope.” Indian Dermatology Online Journal 7, no. 5 (2016): 359. https://doi.org/10.4103/2229-5178.190496.
- Hansraj, Kenneth K. “Assessment of Stresses in the Cervical Spine Caused by Posture and Position of the Head.” Surgical Technology International 25 (November 2014): 277–79. https://pubmed.ncbi.nlm.nih.gov/25393825/.



